Pre-Treatment
QUICK LINKS
Pre-Treatment
– Medication
– Shared Decision Making
– Patient Perspective
– The Multidisciplinary Team
– Family, Friends & Carers
Heart Valve Disease
QUICK LINKS
What is Shared Decision Making?
Shared decision making (SDM) ensures that individuals are supported to make decisions that are right for them. It is a collaborative process through which a clinician supports a patient to reach a decision about their treatment.
The conversation brings together:
- the clinician’s expertise, such as treatment options, evidence, risks and benefits
- what the patient knows best: their preferences, personal circumstances, goals, values and beliefs.
Patient Choice
The NHS vision for Patient Choice by 2020 is that:
- All patients are aware of the choices available to them, particularly where these are legal rights and have the information they need to make meaningful choices,
- All GPs/referrers discuss the different treatment options available to patients, include them in shared decision making, and offer choice to patients,
- All providers make good quality, up to date information about their services available and accept all appropriate patient referrals in line with the NHS Standard Contract,
- All commissioners assess how well choice is working within their CCG and put improvement plans in place to address areas that need strengthening,
- All opportunities to extend the operation of choice beyond existing standards are explored and implemented.
There are pros and cons to each type of surgical procedure and valve replacement, depending on age and lifestyle. You should discuss with your physicians which valve and surgery is most suitable for you.
Due to Patient Choice initiative, patients in the NHS have the right to choose where they are treated but you will need to be referred by your consultant cardiologist or GP.
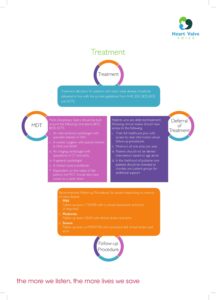
MDT
A Multidisciplinary team, also referred to as a “structural heart team” or simply an “MDT” is a team of health professionals who are experts in heart valve disease and who all have different skill sets.
MDTs play a major role in ensuring that the care a patient receives is patient-centred. Patient-centred care is a fully personalised and individual approach to health care. This means taking into consideration the patient’s wishes, along with all of the other factors surrounding that person’s life and circumstances that affect their health and wellbeing. An MDT is the key to patient-centred care as it involves making the best choices for the patient’s treatment pathway.
Pre-Treatment
QUICK LINKS
Pre-Treatment
– Medication
– Shared Decision Making
– Patient Perspective
– The Multidisciplinary Team
– Family, Friends & Carers
Heart Valve Disease
QUICK LINKS
Patient Story: Ian
Initially, the plan was for open-heart surgery, which I was pretty nervous about. I’m pretty tough and I love life, but the prospect of having your chest opened is scary. I think people think because I’m a dentist by trade I’d be used to stuff like this, but I’m used to standing over the chair, not sitting in it!! Despite my fears and concerns, Dr Jim Hall gave me great confidence and I felt I was in the best hands at James Cook University Hospital. Eventually, we made a shared decision that I would have a TAVI instead.

Read Ian’s story in full…



