Pre-Treatment
QUICK LINKS
Pre-Treatment
– Medication
– Shared Decision Making
– Patient Perspective
– The Multidisciplinary Team
– Family, Friends & Carers
Heart Valve Disease
QUICK LINKS
What is an MDT (Multidisciplinary Team?)
A Multidisciplinary team also referred to as a “structural heart team” or simply an “MDT”, is a team of health professionals who are experts in heart valve disease and who all have different skill sets.
Who is involved?
The team typically includes heart valve surgeons, interventional cardiologists and imaging cardiologists. Surgeons perform open heart operations, interventional cardiologists perform procedures done via the catheter route from the groin, and imaging cardiologists perform and report diagnostic scans of all kinds. There may also be specialist nurses, physiologists and junior doctors/other trainees on the team and a co-ordinator, who may serve as the main point of contact for healthcare professionals and patients alike, depending on local arrangements.
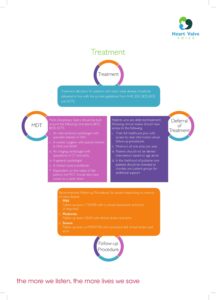
How often do they meet?
MDTs meet regularly to discuss patients’ cases in detail, review their test results and agree a plan of action for the right treatment. The details of the discussion in an MDT meeting include the type and severity of valve disease, the patient’s general health, including any other medical conditions, current medication and potential for rehabilitation and recovery. In the context of the latest guidelines, the MDT will reach a conclusion and make a recommendation for what the group considers to be the best treatment option for each case.
What is their role?
MDTs play a major role in ensuring that the care a patient receives is patient-centred. Patient-centred care is a fully personalised and individual approach to health care. This means taking into consideration the patient’s wishes, along with all of the other factors surrounding that person’s life and circumstances that affect their health and wellbeing. An MDT is the key to patient-centred care as it involves making the best choices for the patient’s treatment pathway.
Why are they important?
The involvement of a number of different healthcare professionals acts as a check and balance, ensuring that the recommendation you receive is truly the best one. While at times the patient may feel that their requests and opinions are being unheard, in actuality it is the opposite, as the main goal of an MDT and patient-centred care is that there is a consensus reached by both clinicians and patient that the agreed upon treatment is ultimately the best for that patient.
Prior to the establishment of MDTs, decisions about patient care were usually made by clinicians working in isolation from one another with little information sharing and often inefficient communication to the patient. Now with help of MDTs, patients can be assured that their treatment and care will be considered by a group of experts with specialist knowledge in the required field, that they will receive the information and support they need to cope with their condition, that there will be continuity of care throughout their treatment pathway, that all of the clinicians will be in continuous communication with one another, that guidelines will be followed and that there will be a more efficient use of time and resources for the benefit of the patient.
What can I do as a patient?
Here are some questions that you, as a patient, might want to ask your doctors about the MDT arrangements in the hospital where you will be assessed and treated for valve disease:
- Do you have an MDT?
- When/how often does the MDT meet?
- When will my case be discussed at MDT
- How/when will I find out the results of the MDT discussion?
- Is there an MDT co-ordinator or someone else who will be my point of contact?
- If I don’t hear anything, how long should I leave it before I contact someone?
Heart Valve Voice’s Gold Standard of Care –
“All MDTs should be made up of the following core team of healthcare professionals: an interventional cardiologist with a specialist interest in TAVI, a cardiac surgeon with a specialist interest in TAVI and SAVR, an imaging cardiologist who specialises in echo and CT, a general cardiologist, and a clinical nurse practitioner. Dependent on the needs of the individual patient, an MDT should also have access to a wider team, including: a care of the elderly physician, a vascular surgeon, a vascular radiologist, a cardiac anaesthetist, and palliative care clinician.”
Pre-Treatment
QUICK LINKS
Pre-Treatment
– Medication
– Shared Decision Making
– Patient Perspective
– The Multidisciplinary Team
– Family, Friends & Carers
Heart Valve Disease
QUICK LINKS



